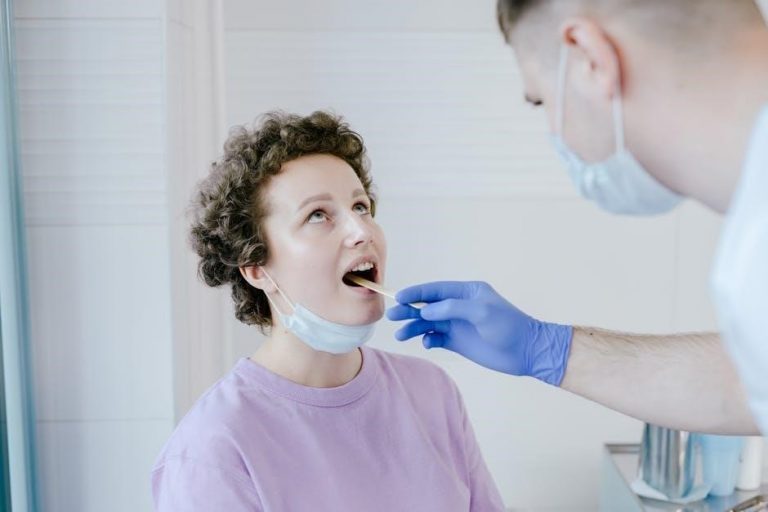
Paediatric clinical examination relies on detailed history and observation‚ as emphasized in resources like “Paediatric Clinical Examination Made Easy”․
Effective techniques‚ illustrated in “Pediatric Physical Examination”‚ are crucial for accurate assessments․
“Examination Paediatrics” guides clinicians through procedures and management of common childhood conditions․
Importance of a Thorough Examination
A comprehensive paediatric clinical examination is paramount for accurate diagnosis and effective patient care․ As highlighted in “Paediatric Clinical Examination Made Easy”‚ simply knowing isn’t enough; clinicians must see enough‚ meticulously observing and gathering information․
This detailed approach‚ supported by resources like “Pediatric Physical Examination”‚ allows for the identification of subtle cues often missed with cursory assessments․ Recognizing family‚ cultural‚ and racial considerations‚ as emphasized in the latter‚ further refines diagnostic accuracy․
A thorough examination‚ guided by texts like “Examination Paediatrics”‚ isn’t merely about identifying illness; it’s about understanding the child’s overall health and well-being‚ forming a strong foundation for appropriate management and intervention․
Overview of the Paediatric Examination Process
The paediatric examination is a systematic process‚ beginning with a detailed history – presenting complaint‚ past medical‚ developmental‚ family‚ and social factors․ Resources like “Examination Paediatrics” emphasize structured history taking․
This is followed by a physical examination‚ progressing from general observation to a head-to-toe assessment․ “Pediatric Physical Examination” provides illustrated guidance on techniques‚ including vital signs and specific system evaluations․
“Paediatric Clinical Examination Made Easy” reminds us of the importance of a friendly demeanour throughout․ The process requires adaptation based on age‚ as techniques differ for infants versus adolescents‚ ensuring accurate and comfortable assessments․
History Taking in Paediatrics
A thorough history‚ encompassing presenting complaints‚ past illnesses‚ development‚ family background‚ and social context‚ forms the foundation of paediatric assessment․
“Examination Paediatrics” highlights its importance․
Presenting Complaint
The presenting complaint is the primary reason a child is brought for medical attention‚ best elicited directly from the child when possible‚ and supplemented by parental observations․
It should be recorded in the parent’s or child’s own words‚ avoiding medical jargon‚ and focusing on the most concerning symptom or issue․
Careful attention to the duration‚ location‚ character‚ and any associated symptoms is vital․
Resources like “Paediatric Clinical Examination Made Easy” emphasize the importance of a focused initial inquiry․
Understanding the context surrounding the complaint – when it started‚ what makes it better or worse – provides crucial early clues․
A clear‚ concise description sets the stage for a comprehensive history․
History of Presenting Illness
Expanding on the presenting complaint‚ the history of presenting illness (HPI) details the chronological development of the problem․
This involves a thorough exploration of the symptom’s onset‚ progression‚ and any modifying factors․
Key elements include detailed questioning about associated symptoms‚ alleviating or aggravating factors‚ and previous episodes․
“Examination Paediatrics” highlights the need to understand the impact on the child’s daily activities․
A clear timeline is essential‚ and parental recall should be carefully elicited‚ acknowledging potential inaccuracies․
The HPI provides the narrative context for the presenting complaint‚ guiding further investigation․
Past Medical History
A comprehensive past medical history (PMH) is vital‚ encompassing previous illnesses‚ hospitalizations‚ surgeries‚ and significant injuries․
Details regarding childhood infections‚ allergies (including reactions)‚ and current medications are crucial․
Immunization status must be meticulously documented‚ noting dates and types of vaccines received․
“Examination Paediatrics” emphasizes the importance of inquiring about chronic conditions like asthma or diabetes․
Previous specialist consultations and their outcomes should also be recorded․
A thorough PMH provides context for the current illness and helps identify potential predisposing factors․
Accurate record-keeping‚ as highlighted in resources‚ is paramount for continuity of care․
Developmental History
A detailed developmental history is essential‚ charting milestones achieved in gross motor‚ fine motor‚ speech‚ and social skills․
Inquire about age of first walking‚ talking‚ and toilet training‚ comparing to expected norms․
Assess current developmental level‚ noting any delays or regressions․
“Paediatric Clinical Examination Made Easy” stresses the importance of a friendly demeanour during this assessment․
School performance‚ if applicable‚ should be reviewed‚ including academic progress and social interactions․
Any concerns raised by parents or caregivers regarding development must be thoroughly investigated;
Understanding developmental trajectories aids in identifying potential neurodevelopmental disorders․
Family History
A comprehensive family history is vital‚ extending to first-degree relatives – parents‚ siblings‚ and grandparents․
Specifically inquire about genetic conditions‚ chronic illnesses (like heart disease‚ diabetes‚ asthma)‚ and any history of sudden infant death syndrome (SIDS)․
Document ethnicity‚ as certain genetic predispositions are more prevalent in specific populations․
“Examination Paediatrics” highlights the importance of understanding chronic paediatric clinical problems within families․
Ask about allergies and sensitivities within the family‚ as these can have a genetic component․
Mental health history in family members should also be noted‚ as these conditions can have a hereditary link․
This information aids in risk assessment and guides further investigation․
Social History
A thorough social history explores the child’s environment and potential psychosocial stressors․
Inquire about the family structure‚ parental education and occupation‚ and socioeconomic status․
Assess the home environment for safety hazards and exposure to toxins‚ like smoke or lead․
Details regarding childcare arrangements and school performance are also crucial․
Explore the child’s social interactions‚ including friendships and involvement in extracurricular activities․
“Pediatric Physical Examination” emphasizes the importance of cultural assessment‚ impacting social context․
Address any concerns regarding emotional well-being‚ behavioral issues‚ or exposure to trauma․
Understanding these factors provides a holistic view of the child’s health and development․

Physical Examination Techniques
Systematic assessment‚ detailed in resources like “Pediatric Physical Examination”‚ involves observation‚ palpation‚ percussion‚ and auscultation․
Illustrated techniques enhance accuracy‚ aiding in identifying normal and abnormal findings․
General Appearance & Observation
Initial observation provides crucial insights before direct interaction․ Assess the child’s overall appearance‚ noting their level of alertness‚ distress‚ and nutritional status․ Observe their spontaneous movements‚ posture‚ and interaction with caregivers․
Look for signs of illness‚ such as pallor‚ cyanosis‚ or respiratory distress․ Note any unusual odors or rashes․ A friendly demeanor‚ as highlighted in “Paediatric Clinical Examination Made Easy”‚ is essential to establish rapport and encourage cooperation․
Consider cultural factors influencing a child’s presentation‚ as emphasized in “Pediatric Physical Examination”․ Careful observation forms the foundation for a focused and effective examination‚ guiding subsequent steps․
Vital Signs Measurement
Accurate vital signs are fundamental to paediatric assessment․ Begin with temperature assessment‚ utilizing appropriate methods for age – tympanic‚ axillary‚ or rectal․ Monitor heart rate and respiratory rate‚ noting rhythm and effort․ Normal ranges vary significantly with age‚ requiring familiarity with paediatric norms․
Blood pressure measurement requires appropriately sized cuffs and careful technique․ Resources like “Examination Paediatrics” provide guidance on interpreting values relative to age and percentile charts․
Document all measurements meticulously‚ recognizing that deviations from normal can indicate underlying pathology․ Consistent monitoring of vital signs is crucial for tracking a child’s condition and response to treatment․
Temperature Assessment
Temperature assessment in paediatrics requires selecting the most appropriate method based on the child’s age and clinical setting․ Rectal temperatures are considered the most accurate for infants‚ while tympanic (ear) measurements are quick and convenient․ Axillary (armpit) readings are non-invasive but less precise․
Understanding normal temperature ranges is vital; variations exist with age and measurement site․ Resources emphasize careful technique to minimize errors․ Document the method used alongside the reading․
Fever is a common presentation‚ but interpreting temperature requires considering the child’s overall clinical picture and activity level․
Heart Rate & Respiratory Rate
Assessing heart and respiratory rates in children differs from adults due to physiological variations․ Heart rate is typically faster in younger children‚ decreasing with age․ Accurate measurement requires counting beats for a full minute‚ especially in infants and toddlers where rhythms can be irregular․
Respiratory rate should be observed without alerting the child to avoid altered breathing patterns․ Normal ranges vary significantly with age․ Observing the effort of breathing – noting any retractions or nasal flaring – is crucial․
These vital signs provide key insights into a child’s cardiopulmonary status and overall well-being․
Blood Pressure Measurement
Blood pressure measurement in children requires appropriately sized cuffs to ensure accuracy; using a cuff that is too large or too small will yield incorrect readings․ Proper technique involves positioning the child comfortably‚ supporting their arm at heart level‚ and selecting the correct cuff size based on arm circumference․
Normal blood pressure values vary significantly with age‚ sex‚ and height percentile․ Reference charts should be consulted to interpret readings appropriately․ Elevated blood pressure requires repeat measurements and further evaluation to rule out underlying conditions․
Accurate blood pressure assessment is vital for identifying cardiovascular risks․
Head-to-Toe Examination
A systematic head-to-toe examination is fundamental in paediatrics‚ beginning with general observation and progressing through each body system․ This approach‚ detailed in resources like “Examination Paediatrics”‚ ensures no area is overlooked․
The neurological assessment includes cranial nerve evaluation‚ motor strength‚ reflexes‚ and assessment of developmental milestones․ Cardiovascular examination focuses on heart sounds‚ murmurs‚ and peripheral pulses․ Respiratory assessment involves auscultation of lung sounds and observation of respiratory effort․
Abdominal palpation checks for organomegaly‚ while musculoskeletal assessment evaluates range of motion and any abnormalities․ This comprehensive approach aids in accurate diagnosis․
Neurological Examination
The paediatric neurological examination requires a tailored approach‚ considering age-related developmental stages․ It begins with observing the child’s alertness‚ spontaneous movements‚ and response to stimuli․ A crucial component is the assessment of cranial nerves‚ testing functions like vision‚ facial movement‚ and hearing․
Motor function is evaluated by observing muscle tone‚ strength‚ and coordination․ Reflexes‚ including primitive reflexes in infants‚ are assessed to identify any neurological deficits․ Observing gait and posture provides further insights․
Careful documentation of findings is essential‚ as highlighted in resources detailing comprehensive paediatric assessments․
Assessment of Cranial Nerves
Evaluating cranial nerves in children demands a systematic approach‚ adapting techniques to their age and cooperation levels․ Olfactory nerve testing is often omitted in young children due to their inability to reliably report smells․ Optic nerve assessment checks visual acuity and fields․
Oculomotor‚ trochlear‚ and abducens nerves are assessed by observing eye movements and pupillary responses․ Facial nerve function is tested by observing facial expressions and taste sensation․ Acoustic nerve evaluation assesses hearing‚ while glossopharyngeal and vagus nerves are checked via gag reflex;
Thorough documentation of each nerve’s function is vital for accurate neurological diagnosis‚ as emphasized in paediatric examination guides․
Motor Function & Reflexes
Assessing motor function in children involves observing spontaneous movements‚ muscle tone‚ and strength․ Observe for asymmetry or limitations in movement․ Strength is assessed by testing muscle groups against resistance‚ adapting to the child’s age and willingness to cooperate․
Reflexes‚ including primitive reflexes (present at birth‚ disappearing with development) and deep tendon reflexes (biceps‚ triceps‚ brachioradialis‚ patellar‚ Achilles)‚ are elicited and graded․ Absent‚ diminished‚ or exaggerated reflexes can indicate neurological issues․
Careful evaluation of motor skills and reflexes‚ guided by resources on paediatric examination‚ is crucial for identifying developmental delays or neurological abnormalities․
Cardiovascular Examination
A thorough cardiovascular examination begins with observation for signs of distress‚ cyanosis‚ or edema․ Palpation identifies the point of maximal impulse (PMI) and assesses for thrills․ Peripheral pulses – brachial‚ radial‚ femoral‚ dorsalis pedis‚ and posterior tibial – are palpated and graded for strength and symmetry․
Auscultation of heart sounds reveals rate‚ rhythm‚ and any murmurs․ Note the location‚ timing‚ and characteristics of any murmurs․ Resources like “Paediatric Clinical Examination Made Easy” emphasize careful listening․
Accurate assessment‚ guided by illustrated handbooks‚ helps detect congenital heart defects or acquired cardiac conditions․
Auscultation of Heart Sounds
Careful auscultation of heart sounds is fundamental․ Utilize both the diaphragm and bell of the stethoscope‚ listening at the mitral‚ tricuspid‚ aortic‚ and pulmonic areas․ Assess the rate and rhythm‚ noting any irregularities․ Identify S1 and S2 sounds‚ and listen for extra sounds like S3 or S4․
Murmurs‚ if present‚ are characterized by timing (systolic or diastolic)‚ location‚ intensity‚ pitch‚ and quality․ Resources like “Paediatric Clinical Examination Made Easy” stress the importance of detailed description․
Distinguishing innocent murmurs from pathological ones requires experience and a systematic approach‚ aided by illustrated guides․
Palpation of Peripheral Pulses
Palpate peripheral pulses bilaterally‚ including radial‚ brachial‚ femoral‚ dorsalis pedis‚ and posterior tibial pulses․ Assess pulse rate‚ rhythm‚ and amplitude‚ comparing sides for symmetry․ Note any diminished or absent pulses‚ which may indicate vascular compromise․
In infants‚ brachial and femoral pulses are often the most readily palpable․ Accurate assessment is crucial‚ as highlighted in resources detailing paediatric clinical examination techniques․
Consider age-related variations; weaker pulses may be normal in smaller children․ Documentation of pulse characteristics is vital for comprehensive evaluation‚ as emphasized in clinical guides․
Respiratory Examination
Begin with observation of respiratory effort‚ noting any signs of distress like nasal flaring‚ intercostal retractions‚ or use of accessory muscles․ Auscultate lung sounds systematically‚ comparing both sides for breath sounds‚ wheezes‚ crackles‚ or diminished air entry․
Assess respiratory rate and rhythm‚ recognizing age-specific norms․ Resources on paediatric clinical examination emphasize the importance of identifying abnormal breath sounds․
Percussion can help identify areas of consolidation or effusion․ Document findings accurately‚ as detailed respiratory assessment is crucial for diagnosing conditions like pneumonia or asthma․
Auscultation of Lung Sounds
Systematically auscultate all lung fields‚ comparing left to right‚ anteriorly‚ posteriorly‚ and laterally․ Utilize both the diaphragm and bell of the stethoscope‚ listening for breath sounds – vesicular‚ bronchial‚ or bronchovesicular – noting any variations․
Identify adventitious sounds such as wheezes (high-pitched whistling)‚ crackles (fine or coarse bubbling)‚ or rhonchi (low-pitched rattling)․ Resources on paediatric examination highlight the importance of differentiating these sounds․
Document the presence‚ location‚ and characteristics of any abnormal sounds‚ as these findings are critical for diagnosing respiratory illnesses in children․
Observation of Respiratory Effort
Carefully observe the child’s respiratory pattern‚ noting the rate‚ rhythm‚ and depth of breathing․ Look for signs of increased work of breathing‚ such as nasal flaring‚ intercostal retractions (pulling in of the skin between the ribs)‚ or subcostal retractions (pulling in of the skin below the ribs)․
Assess for accessory muscle use – the child using neck or abdominal muscles to assist breathing․ Cyanosis (bluish discoloration of the skin) indicates low oxygen levels and requires immediate attention․
Document any observed abnormalities‚ as these are crucial indicators of respiratory distress and guide clinical decision-making‚ as emphasized in paediatric examination guides․
Abdominal Examination
Begin with inspection‚ noting the contour‚ distension‚ and visible peristalsis․ Auscultate bowel sounds in all four quadrants‚ listening for presence‚ absence‚ or character (normal‚ hyperactive‚ hypoactive)․ Remember to use a diaphragm for high-pitched sounds and a bell for low-pitched sounds․
Proceed to palpation‚ starting with light palpation to assess for tenderness‚ guarding‚ or muscle rigidity․ Then‚ perform deep palpation to identify any organomegaly (enlarged organs)‚ masses‚ or abnormalities․
Document findings accurately‚ as abdominal examination is vital for diagnosing various paediatric conditions‚ as detailed in comprehensive examination resources;
Auscultation of Bowel Sounds
Begin by placing the diaphragm of the stethoscope lightly on the abdomen in all four quadrants․ Listen for the characteristic gurgling sounds produced by peristalsis – the muscular contractions moving intestinal contents․
Normal bowel sounds are typically irregular and occur several times per minute․ Hyperactive bowel sounds may indicate early obstruction or gastroenteritis‚ while hypoactive or absent sounds could suggest ileus or late-stage obstruction․
Document the presence‚ absence‚ frequency‚ and character of bowel sounds accurately․ This is a crucial step in the abdominal examination‚ as highlighted in paediatric clinical examination guides‚ aiding in differential diagnosis․
Palpation for Organomegaly
Gentle‚ yet systematic‚ palpation of the abdomen is essential to detect organomegaly – enlargement of abdominal organs like the liver‚ spleen‚ or kidneys․ Begin with light palpation to assess for tenderness‚ then progress to deeper palpation using both hands․
The liver edge may be palpable below the right costal margin‚ while the spleen is typically felt in the left upper quadrant․ Note the size‚ shape‚ consistency‚ and any tenderness of any palpable organs․
Accurate documentation of findings‚ as emphasized in paediatric clinical examination resources‚ is vital for diagnosis․ Palpation helps identify potential causes of abdominal distension or pain․
Musculoskeletal Examination
A thorough musculoskeletal examination in paediatrics involves observation‚ palpation‚ range of motion assessment‚ and assessment of muscle strength․ Observe for asymmetry‚ swelling‚ or deformities․ Palpate joints and bones for tenderness or masses․
Evaluate active and passive range of motion in all major joints‚ noting any limitations or pain․ Assess muscle strength by testing key muscle groups against resistance‚ comparing bilaterally․
Resources like “Paediatric Clinical Examination Made Easy” highlight the importance of a systematic approach․ Consider developmental milestones and age-related variations during the examination․
Specific Considerations in Paediatric Examination
Age‚ cultural background‚ and physiological differences significantly impact the paediatric examination; sensitivity and adaptation are key‚ as noted in resources․
Age-Related Anatomical & Physiological Differences
Paediatric patients exhibit distinct anatomical and physiological characteristics that necessitate tailored examination techniques; Infants possess a relatively larger head circumference and shorter limbs compared to adults‚ influencing auscultation points and palpation strategies․
Respiratory rates are naturally higher in children‚ and their chest walls are more compliant‚ impacting breath sound assessment․ Cardiovascular systems also differ; heart rates vary significantly with age‚ and peripheral pulses may be more difficult to palpate in neonates․
Furthermore‚ developmental milestones influence a child’s ability to cooperate during the examination․ Understanding these age-specific variations‚ highlighted in resources like “Pediatric Physical Examination”‚ is paramount for accurate clinical evaluation and diagnosis․
Adapting Techniques for Different Age Groups
Paediatric clinical examination requires adapting techniques based on the child’s developmental stage․ With infants‚ gentle handling and observation during feeding or quiet moments are essential․ Toddlers may require distraction or parental involvement to facilitate cooperation․
School-aged children can understand simple explanations and participate more actively‚ while adolescents may appreciate privacy and direct communication․ Auscultation and palpation methods must be modified; for example‚ using a pediatric stethoscope head and applying lighter pressure․
Resources like “Paediatric Clinical Examination Made Easy” emphasize a friendly demeanour and age-appropriate communication․ Recognizing these nuances ensures a thorough and less stressful examination experience for both the child and the clinician․
Cultural Sensitivity in Examination
Paediatric clinical examinations must be conducted with profound cultural sensitivity․ Family and cultural assessment are increasingly vital‚ as highlighted in “Pediatric Physical Examination: An Illustrated Handbook”․ Understanding diverse beliefs about health‚ illness‚ and pain expression is crucial․
Direct eye contact‚ physical touch‚ and questions about sensitive topics may be interpreted differently across cultures․ Clinicians should be aware of potential language barriers and utilize qualified interpreters when needed․
Respecting family dynamics and involving caregivers appropriately demonstrates cultural humility․ Recognizing these factors fosters trust and improves the accuracy of the examination‚ leading to better healthcare outcomes for all children․
Documentation and Interpretation
Accurate record-keeping of findings is essential․ Distinguishing normal from abnormal results‚ informed by examination skills‚ aids diagnosis and guides appropriate paediatric care․
Accurate Record Keeping
Meticulous documentation forms the cornerstone of effective paediatric care‚ ensuring continuity and facilitating informed decision-making․ Records should be comprehensive‚ detailing all observations from the history and physical examination‚ including vital signs‚ developmental milestones‚ and any pertinent family or social factors․
Clarity and objectivity are paramount; avoid subjective interpretations and instead focus on factual descriptions․ Utilize standardized charting systems where available to promote consistency․
Electronic health records (EHRs) offer advantages in terms of accessibility and legibility‚ but require diligent data entry and security protocols․
Remember‚ the clinical record serves as a legal document and a vital communication tool between healthcare professionals․
Identifying Normal vs․ Abnormal Findings
Distinguishing between normal variations and pathological findings is central to paediatric clinical examination․ Age-related anatomical and physiological differences necessitate a strong understanding of developmental norms․ Resources like “Pediatric Physical Examination” emphasize recognizing expected findings at each stage․
Consider the child’s gestational age‚ growth patterns‚ and genetic predisposition when interpreting examination results․ Subtle deviations from the norm may indicate underlying issues‚ requiring further investigation․
A systematic‚ head-to-toe approach aids in identifying abnormalities․
Clinical judgement‚ combined with a thorough understanding of paediatric medicine‚ is crucial for accurate interpretation and appropriate management․
Utilizing Examination Findings for Diagnosis
Examination findings‚ when integrated with a comprehensive history‚ form the cornerstone of accurate paediatric diagnosis․ “Examination Paediatrics” highlights aligning findings with potential clinical problems․
A systematic approach‚ as advocated in “Paediatric Clinical Examination Made Easy”‚ allows for pattern recognition and differential diagnosis․ Consider the presenting complaint and history of present illness alongside physical exam results․
Utilize “Pediatric Pearls” from illustrated handbooks to refine diagnostic skills․
Investigations should be guided by examination findings‚ avoiding unnecessary tests․ Clinical judgement and experience are vital for formulating a precise diagnosis and treatment plan․